It recently occurred to me that I’ve now been coping and living with my cancer for more than 10% of my life. 12.86%, to be precise, which equates to more than an eighth of my time on Earth. And I tend not to talk about my cancer story much on here. Not least because I set up this site specifically to distract me from the posts I make on my Cancer Dad site. But the reality is that cancer has been a huge part of my life, so I thought it right to make a summary of my cancer story so far.
My cancer story started in 2014, when I was 43…
In reality, my cancer story started much earlier than that, I just hadn’t noticed it yet. Or, perhaps, I hadn’t wanted to notice it yet! With hindsight, there were plenty of increasingly obvious signs and symptoms, which I simply refused to acknowledge. Or, at least, to associate them with anything worse than diet and exercise.
In the end, a combination of extreme fatigue and a, very noticeable change in bowel habit, drove me to see my doctor. Which is how, in late January 2014, I made the first step in my cancer story: a digital rectal examination from my GP.
Despite telling me it was only haemorrhoids, my GP still referred me to see a specialist at the hospital, who carried out a rigid sigmoidoscopy. This is an endoscopy process that allows the inside of the rectum to be imaged. The result of which, was the discovery of ‘blood above the haemorrhoid line’. A diagnosis which meant that something else had to be in play, so I was sent for a colonoscopy.
You go 43 years with one way traffic, then three things arrive at once that want to go in the other direction…
During the colonoscopy, it became very clear, very quickly that I had bowel cancer. I could see the screen that the consultant was using to navigate the colonoscope (an excellent word, by the way). There were fronds of white tissue that weren’t supposed to be there. Even I, armed only with an A Level in Biology, could tell that.
So, as he worked, I asked the consultant about them. This seemed to catch him somewhat off guard, but then I’d opted not to have the sedative, so I could play hockey the next day. Priorities are important… Anyway, for whatever reason, the consultant was quite forthcoming with his answers and confirmed that, yes, we were looking at rather a lot of cancer.
This news, despite being so bloody obvious, still managed to catch me off guard. I actually shut up for a while, as I processed the information. By the time he’d finished, I’d come to the conclusion that, ‘This is bad!’ A sparkling display of intellect, I think you’ll agree.
But, mentally speaking, this was the actual start of my cancer story. Prior to this point I’d been totally in denial of my situation. Even after the results of the rigid sigmoidoscopy, I’d grasped at the straw that it was something else. Like Ulcerative Colitis, which is what the footballer Darren Fletcher has. But, no: it was cancer. And it was time to face the music.

did not mean that that the rest of my life story had to stop.
But accepting things for myself was the least of the problem. I had to find the right way to tell my friends and family. This resulted in a very difficult and complicated decision making process, of who to tell what, and when…
Julie was at the hospital with me, so heard the official confirmation in the meeting after the colonoscopy. She already knew. She’d seen the signs and symptoms in me, and come to the obvious conclusion, in a way that I had avoided. Thus started Julie’s new position as, Rock of Stability in the Midst of Chaos and Uncertainty. Something she never asked for, or wanted, but still does heroically anyway.
We decided to immediately share the news with our parents and siblings. They would want to know. Just as, had it been the other way around, we would have wanted to know. However, we chose to delay telling the girls anything at that point. They were only 10 and 12, so we decided to wait until we got the scan and biopsy results back, before telling them anything. Better, we thought, to get the whole story ourselves, before burdening them with such life-altering news.
And the meeting where I got the scan and biopsy results back, was a tough one. The scans indicated seven tumours on my liver, and activity in my lymph nodes. The biopsies confirmed that the primary tumours in my bowel were, indeed, malignant. All of which meant that I had a five-year survival rate of about 3%. When this news was delivered, I could feel the world closing in. It felt like I could hear a gale howling towards me. The consultant noticed the change in me and asked if I was okay, which allowed me to snap out of it. It was a very strange sensation.
At the end of the meeting, I was told that I’d be called in for a PET-CT scan to have a closer look.
While we kept the survival rate stuff to ourselves, the rest had to be shared with the families again. Worse still, we had to tell the girls that I had cancer and that I’d need surgery and chemotherapy. This process was about the hardest thing that I went through. I wouldn’t wish it on anyone.
It was also around this time that I started sharing my cancer story on Facebook. It seemed the best way of keeping everyone informed. That way, when I saw someone I knew, there was a good chance they knew where I was. They could then choose to talk about it, or not. Easier for me. Easier all round.
The PET-CT scan revealed that only two of the liver tumours were cancer. The others were hemangiomas: stretch marks, if you will. It also turned out that only one of the lymph nodes was affected, meaning surgery was definitely an option. All of which meant that my five-year survival rate jumped to 30%.
Hell, yeah!
And I’m serious about this excitement. I was genuinely thrilled to be told that I had a one in three chance of making it to the five-year mark. Thrilled, because it was so much better than what my previous situation had been. I did reflect at the time, though, how strange life can be. To actually feel happy when you’re told that you’ll probably die before you’re 50. Because it’s an improvement on, you’ll almost certainly die before you’re 50… It’s astonishing what you can get used to.
And, with this new sense of relief, came the first meeting with my oncologist, who then became the person in charge of my case. It is still the oncologist that I go to see about my scans, and it is the oncologist who liaises with the other medical professionals to decide my treatment. It was through the oncologist that the treatment phase of cancer story began.
The treatment that was agreed upon was:
- 3 months of chemotherapy;
- bowel resection surgery, to remove the primary tumour;
- liver resection surgery, to remove the metastases;
- another 3 months of chemo, then;
- cancer free…

So I had 4 three-weekly cycles of IV Oxaliplatin, along with Capecitabine in tablet form. This was a draining process that left me increasingly immobile due to the side effect of nausea. The knock on effect of which, was that I started piling on weight, something that would take years to rectify. And then there was the chemo-brain… The chemotherapy ravaged my memory and stomped on my ability to process information: to think laterally. It’s unlikely that I’ll ever get back to the way I was.
After the first three months of chemo, I had a scan to see how well it was doing. Not well at all, as it turned out. The tumours hadn’t got any bigger, but that was about all. As far as I was concerned, this was not a great return on all the side effects that I was experiencing. Still, at least it was time for the surgeries…
They started with the liver resection, on 9th September 2014. I still don’t know why they chose to do this one first but, Hey Ho! After the liver resection, I struggled with complications. First there were collections on the liver that no one could decide what to do about. Then, on 19th September I was hospitalised with rigors: an infection-related uncontrollable shaking.
A development that put paid to the bowel resection surgery that had been scheduled for 24th September.
Instead I got a lot of blood tests and some ultrasound scans on the site of the liver resection. The results of which sent me back to hospital for a couple of days on the 14th October. And again on the 24th. Somewhere during all these delays, the tumours got big enough to completely obstruct my bowel, which ruptured in protest…
This rupture in my bowel was discovered on 28th October 2014, during the bowel resection surgery itself. Which, I’m told, made the surgery considerably more difficult than anticipated. Apparently, I was full of shit… Julie could have told them that!
Anyway, the bowel rupture also made my recovery a much lengthier process. Not least because it meant that I needed a stoma and a colostomy bag, to avoid further infection. And, although I make light of it now, the bowel rupture nearly killed me. How I got away without peritonitis, I really don’t know. Given the amount of serous fluid that leaked through my stitches, it must have been a close-run thing.
When I was well enough, and despite the Oxilaplatin and Capeciabine regime not being that effective on me, it was back on the chemo. I completed the course by doing another 4 cycles over the next three months.
There was one brief moment of excitement, during this second round of chemotherapy…
On New Year’s Eve, 2014, I found myself struggling to breathe. This is rarely a good thing, so we decided that a trip to the hospital might be in order. It turned out that I’d had a deep vein thrombosis, which had led to bilateral pulmonary emboli. Basically, I had blood clots on both lungs. And that’s how I ended up on blood thinners for six months.
Anyway, back to the chemo. At the end of the course, I was given another scan, and declared cancer free!
This was in April 2015, a little over a year into my cancer story.
It was very carefully explained to me, at the time, that ‘cancer free’ is not the same as ‘cured’. What ‘cancer free’ really means is: ‘We’ve cut out everything we could find and there’s nothing left that is big enough to be identified from the scans’. Scans can only distinguish objects above about 5mm (¼ inch) in size. Anything less just gets lost in the background noise. Meaning there could be any number of 2mm and 3mm tumours, growing away.

Well, with the benefit of hindsight: exercise. I should have ‘celebrated’ with diet and exercise…
Taking everything into account, it seemed utterly implausible that my cancer story was actually over. As such, being told that I was now fine, and to get on with my life, just didn’t sit right. I immediately sank into depression. So I saw my GP and was put on Citalopram, which I stuck with for the next two years. I also sought counselling, where I was told that I was struggling with an adjustment disorder.
I’m going to go out on a limb, here, and say that having a colostomy bag probably didn’t help much either… That damn bag could fart at the worst possible moments. Sometimes I was sure it did it on purpose. Surely the timings can’t all have been coincidence…!?
Anyway, now that I was cancer free, at least I could do something about the colostomy bag. I needed to have a follow-up scan after six months, at which point I could have the reversal surgery. So the reversal was booked in for October 6th, and I was instructed to lose some weight in the meantime.
I lost the weight, then had my scans. And, on the day before my reversal surgery, I got a call to say the cancer was back in my liver. I’d had a recurrence. So the reversal surgery was off. Instead, I was given another liver resection, on 6th December 2015, up in Bristol. This particular surgery led to a bit of light pneumonia. Nothing to write home about, more like ticking another condition off the list.
Or so I thought…
I eventually made it home on the 12th. But, on the 17th of December, I was in the local hospital with more breathing issues. These stemmed from a pleural effusion, which was more tiring than anything. But, because of the underlying pneumonia, I was kept in hospital until the 21st. Poor Julie had to do all of the Christmas preparations, as well as go to work and look after the girls.
This seems a good a point as any to make clear that cancer doesn’t just happen to the patient, it happens to the whole family. And it is often the carers who get it worst. All the patient has to do is get on with their treatment. The carers have to deal with everything else. Including not being able to talk to the patient about the Hell the carer is going through, because they feel the patient is going through enough.
I probably don’t say it enough, but Julie is amazing.
The follow-up scans for the recurrence, in February 2016, showed… another recurrence.
More tumours in the liver, plus a shiny new one in the lung. Metastases in multiple systems is not a good look. Consequently, my cancer story reached a new chapter: I was moved from curative to palliative care. I was officially terminally ill, and told I could expect to live another two to three years. A development which led to another set of incredibly tough conversations.
It also meant a return to chemotherapy, but of a different type. This time I was given IV Cetuximab and Irinotecan with Fluorouracil (5-FU) delivered, via pump, through a PICC line over 48 hours. It was a 6 month treatment involving 12, two-weekly cycles.
This added up to:
- A semi-permanent tube in my arm (PICC line)
- A hole in my abdomen (stoma)
- Looking like an extra from The Walking Dead (courtesy of the Irinotecan)
- Oh, I also had a sizable hernia, around the site of the stoma
- And I was still taking a kicking from the depression…
Julie could barely keep her hands off me!
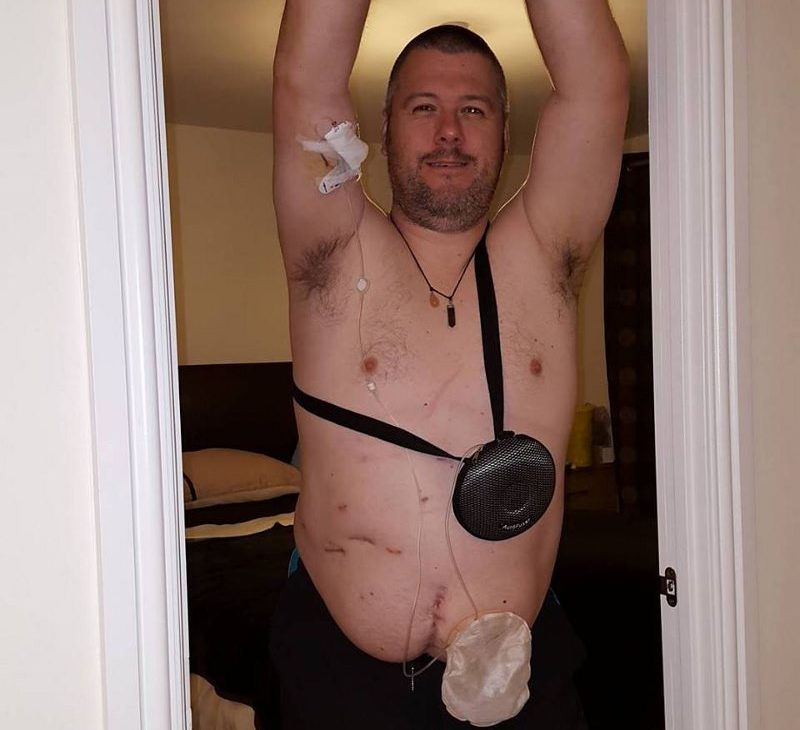
But, I finished the treatment in September 2016 and waited for the scans, the results of which would tell me how long I had. If the tumours came straight back across multiple systems, time was short. If only one tumour came back, then I could soldier on for a while…
Well, the scans came back clean!
I was, once again, cancer free.
Time to make the most of it.
In January 2017, I came off my Citalopram. I just didn’t feel it was working for me any more. The plan was to go onto another type of anti-depressant, but you have to wean yourself off the one before you start the next. Well, I decided not to start the next one. I wanted to see if I could cope without anti-depressants.
To start with, it was rubbish. I could feel all my emotions again but I’d got out of the habit of managing them. It was like being a teenager! Fortunately, that didn’t go on for too long. And, after a couple of weeks, I concluded that, yes: I could cope without the anti-depressants.
And I haven’t needed them since.
In March 2017, I finally got my stoma reversal. But I lost the last surviving bit of my belly button, to a huge abdominal scar, in the process. To my mind, though, this was a small price to pay.
However, over the next couple of months, that scar tissue tightened up. As scar tissue tends to do. It tightened up right down the middle of my abdomen. My rather flabby abdomen… Look, what I’m trying to say, here, is that I ended up with a belly-but. It now looks like I have arse cheeks on my abdomen. Frankly, I’m glad the belly button is gone, otherwise the picture would be complete…!
Still worth it, though.
Especially after I got the hang of using the toilet again. Adult nappies turn out to be horribly sweaty. At least I only felt the need to wear them for the first couple of weeks. And, thankfully, no accidents occurred.
My next two scans, in April and August 2017, came back clear. In fact, for the whole of 2017 my cancer story was effectively on pause. I did have a bought of depression over summer, but worked my way through it with a bit of counselling. I also had a colonoscopy, which had no bad news to reveal.
Yep, 2017 was a good year.
2018, on the other hand, sucked!
In February 2018, the scans reveled that I had a new tumour on my liver. And the one on my lung was back. Therefore, my third recurrence also involved multiple-system metastases. I prepared myself for some bad news regarding the treatment, but, no: surgery was on, despite the locations. And, maybe because of this, I avoided sinking back into depression.

I wish these things could wait until March so I could actually relax and enjoy these ski trips.
On May 2nd I had the liver resection. This time it all went well. I’m not even sure I got any new scars, they just went back in through some of the old ones. What’s the point of surgeries, if you don’t have new scars to show for it?!
I was then sent for a PET/CT scan, to confirm the position of the remaining tumour, prior to the lung surgery. And it was at this point that another fly was added to the ointment. The PET scan showed a hotspot on my Thyroid.
Well… damn!
The news about the thyroid was something of a shock and left me all shook up (uh huh huh). But it quickly led to an ultrasound scan, which confirmed that there was something there. So they did a (remarkably painful) needle aspiration and managed to get some cells. The doctor said that it was too solid to be a cyst and probably too diffuse to be cancer. He said that it certainly wasn’t related to my bowel cancer, which was one good thing.
While the experts pondered the issue of my Thyroid, the thoracic team in Bristol took care of my lung. On July 11th 2018, I had keyhole surgery to cut out a portion of my left lung. Not too much, and not enough to noticeably impact on my lung capacity. Before the surgery, I was able to max out the lung capacity flow meter. After the surgery I was still able to max out the flow meter. That’s good enough for me.
And I definitely got some new scars from this surgery.
And then attention turned back to my Thyroid. The principle seemed to be that it was easier to remove a whole half of the Thyroid, instead of just the hotspot. So, on 10th September 2018, that’s exactly what they did. Another new scar! And, this time, a new medication as well. I’ll need to take a daily thyroxine tablet for the rest of my life. No big deal.
As for the hotspot? That turned out to be nothing.
The follow-up scans were refreshingly clear. As were the ones after that. In fact, I had another whole year off from my cancer story in 2019. We made the most of the break and moved house.
And it was only a break, because my fourth recurrence started in February 2020. We’re back in the liver again. This time in lobe 2. That’s the bit round the front of your chest, on the left: close to the heart and the stomach.
Thankfully, my oncologists, consultants and surgeons are all used to this type of thing now. The conversation went something like this:
Me – “Surgery?”
Oncologist – “Surgery!”
Sadly, our conversation was rudely interrupted by a third party:
COVID-19 – “No surgery for you, sunshine!”
As I’ve said before, I think that cancelling cancer surgeries during the Coronavirus Lockdown was a mistake. So I won’t get into that again here. Regardless of the reason, about a week before I would have had my surgery, all surgeries were cancelled, and that was that.

There’s a ginger kitty in there, somewhere!
But I got lucky. Probably because I have private health cover… Either way, I was offered a course of SABR Radiotherapy treatment at the BRI, up in Bristol. SABR is not as effective as surgery, but still has an 80% success rate. Which, I’m sure you’ll agree, is an awful lot better than nothing. So I accepted the treatment. And, in May 2020, I had five rounds of SABR.
I felt guilty doing so and I still feel guilty now. What if, by taking the treatment, someone else went without? I’m aware that, at the time of the treatment, the private sector was being controlled by the NHS. So, this should mean that proper triage rules are in place. That all treatments were offered in accordance with need, across both parts of the system. But I’ll never know for sure.
It’s something that I’m going to have to live with…
How long I have to live with it, is anyone’s guess.
My prognosis is still that I have two to three years left to live. It’s an ongoing thing that will only make sense in retrospect. There’s no reason that the clock didn’t start ticking in February, when I got told of my latest recurrence…
Mind you, there’s no reason that it did. After all, this is the fifth time in my cancer story that I’ve been told that I’ve got cancer. And who ever said, “Fifth time’s the charm?!”
No one, that’s who.
So, my plan is to keep on keeping on, and wait to see what the scan results in July have to say.
I just felt that my cancer story has become such a major part of my life, that I needed to address it here. My cancer story is part of the larger story of my life, and I need to own that.
And part of owning it, is talking about it.
Something that I now have done…

6 thoughts on “My Cancer Story So Far”
Hey Paul, hope you’re doing good . Did you get your scan results ?
Hi Somdatta,
Yes, thank you, my results are back. They show that the radiotherapy has reduced the size of my liver tumour by about 25%, which is good news. The scans also confirm that there are no additional tumours anywhere else, which is even better. Now it’s just a case of getting a date for some surgery to get rid of the liver tumour altogether. Which will be the best thing of all.
All the best,
Paul
Paul,
Thanks for the story. I am from the United States and I am dealing with stage 4 colon cancer.
Your story helps me. As the saying goes “misery loves company”.
Good luck to you and your family!
Hi Dan,
Really sorry to hear that you’re having to go through it as well. I’m here if you want to chat.
I’m happy to hear that you’ve found my story helpful. It’s nice to know something positive has come from my experiences.
All the best to you and yours,
Paul
Hi Paul,
It’s so great a news ! Have you been able to get a date for surgery yet, for the removal of the tumor in the liver ? Eager to hear from you.
Best wishes 🙂
Hello Somdatta,
Thanks for your support.
Things have taken an unexpected twist with the surgery, in that there is no surgery…
But this is a good thing. My most recent scans were unable to pick out any obvious tumours on my liver. As such, the surgeon couldn’t do any surgery, because he couldn’t see anything to remove. And the reason for that was that the SABR radiotherapy that I had last May has kept working in the background, slowly eating away at the cancer cells. And, now, it seems all the cancer cells are gone.
You’ve got to be happy with that.
My next scans are in the Autumn, and even if the cancer does come back, I’ve had a nice summer off.
All the best,
Paul